Author: Madeleine R. Estryn-Béhar
Ergonomics is an applied science that deals with the adaptation of work and the workplace to the characteristics and capabilities of the worker so that he or she may perform the duties of the job effectively and safely. It addresses the worker’s physical capacities in relation to the physical requirements of the job (e.g., strength, endurance, dexterity, flexibility, ability to tolerate positions and postures, visual and auditory acuity) as well as his or her mental and emotional status in relation to the way the work is organized (e.g., work schedules, workload and work-related stress). Ideally, adaptations are made to the furniture, equipment and tools used by the worker and to the work environment to enable the worker to perform adequately without risk to himself/herself, co-workers and the public. Occasionally, it is necessary to improve the worker’s adaptation to the job through, for example, special training and the use of personal protective equipment.
Since the mid 1970s, the application of ergonomics to hospital workers has broadened. It is directed now at those involved in direct patient care (e.g., physicians and nurses), those involved in ancillary services (e.g., technicians, laboratory staff, pharmacists and social workers) and those providing support services (e.g., administrative and clerical personnel, food service staff, housekeeping staff, maintenance workers and security staff).
Extensive research has been conducted into the ergonomics of hospitalization, with most studies attempting to identify the extent to which hospital administrators should allow hospital personnel latitude in developing strategies to reconcile an acceptable workload with good quality of care. Participatory ergonomics has become increasingly widespread in hospitals in recent years. More specifically, wards have been reorganized on the basis of ergonomic analyses of activity undertaken in collaboration with medical and paramedical personnel, and participatory ergonomics has been used as the basis for the adaptation of equipment for use in health care.
In studies of hospital ergonomics, workstation analysis must extend at least to the departmental level—the distance between rooms and the amount and location of equipment are all crucial considerations.
Physical strain is one of the primary determinants of the health of HCWs and the quality of care that they dispense. This being said, the frequent interruptions that hinder care-giving and the effect of psychological factors associated with confrontations with serious illness, ageing and death must also be addressed. Accounting for all these factors is a difficult task, but approaches focusing only on single factors will fail to improve either working conditions or the quality of care. Similarly, patients’ perception of the quality of their hospital stay is determined by the effectiveness of the care they receive, their relationship with physicians and other personnel, the food and the architectural environment.
Basic to hospital ergonomics is study of the sum and interaction of personal factors (e.g., fatigue, fitness, age and training) and circumstantial factors (e.g., work organization, schedule, floor layout, furniture, equipment, communication and psychological support within the work team), which combine to affect the performance of work. Precise identification of the actual work performed by health care workers depends on ergonomic observation of entire workdays and collection of valid and objective information on the movements, postures, cognitive performance and emotional control called upon to satisfy work requirements. This helps to detect factors that may interfere with effective, safe, comfortable and healthy work. This approach also sheds light on the potential for workers’ suffering or taking pleasure in their work. Final recommendations must take the interdependence of the various professional and ancillary personnel attending the same patient into account.
These considerations lay the groundwork for further, specific research. Analysis of strain related to the use of basic equipment (e.g., beds, meal carts and mobile x-ray equipment) may help clarify the conditions of acceptable use. Measurements of lighting levels may be complemented by information on the size and contrast of medication labels, for example. Where alarms emitted by different intensive-care-unit equipment can be confused, analysis of their acoustic spectrum may prove useful. Computerization of patient charts should not be undertaken unless the formal and informal information-support structures have been analysed. The interdependence of the various elements of the work environment of any given caregiver should therefore always be borne in mind when analysing isolated factors.
Analysis of the interaction of different factors influencing care—physical strain, cognitive strain, affective strain, scheduling, ambience, architecture and hygiene protocols—is essential. It is important to adapt schedules and common work areas to the needs of the work team when attempting to improve overall patient management. Participatory ergonomics is a way of using specific information to bring about wide-ranging and relevant improvements to the quality of care and to working life. Involving all categories of personnel in key stages of the search for solution helps ensure that the modifications finally adopted will have their full support.
Working Postures
Epidemiological studies of joint and musculoskeletal disorders. Several epidemiological studies have indicated that inappropriate postures and handling techniques are associated with a doubling of the number of back, joint and muscle problems requiring treatment and time off the job. This phenomenon, discussed in greater detail elsewhere in this chapter and Encyclopaedia, is related to physical and cognitive strain.
Working conditions differ from country to country. Siegel et al. (1993) compared conditions in Germany and Norway and found that 51% of German nurses, but only 24% of Norwegian nurses, suffered lower-back pain on any given day. Working conditions in the two countries differed; however, in German hospitals, the patient-nurse ratio was twice as high and the number of adjustable-height beds half that in Norwegian hospitals, and fewer nurses had patient handling equipment (78% versus 87% in Norwegian hospitals).
Epidemiological studies of pregnancy and its outcome. Because the hospital workforce is usually predominantly female, the influence of work on pregnancy often becomes an important issue (see articles on pregnancy and work elsewhere in this Encyclopaedia). Saurel-Cubizolles et al. (1985) in France, for example, studied 621 women who returned to hospital work after giving birth and found that a higher rate of premature births were associated with heavy housekeeping chores (e.g., cleaning windows and floors), carrying heavy loads and long periods of standing. When these tasks were combined, the rate of premature births was increased: 6% when only one of these factors was involved and up to 21% when two or three were involved. These differences remained significant after adjustment for seniority, social and demographic characteristics and professional level. These factors were also associated with a higher frequency of contractions, more hospital admissions during pregnancy and, on average, longer sick leave.
In Sri Lanka, Senevirane and Fernando (1994) compared 130 pregnancies borne by 100 nursing officers and 126 by clerical workers whose jobs presumably were more sedentary; socio-economic backgrounds and use of prenatal care were similar for both groups. Odds-ratios for complications of pregnancy (2.18) and preterm delivery (5.64) were high among nursing officers.
Ergonomic Observation of Workdays
The effect of physical strain on health care workers has been demonstrated through continuous observation of workdays. Research in Belgium (Malchaire 1992), France (Estryn-Béhar and Fouillot 1990a) and Czechoslovakia (Hubacova, Borsky and Strelka 1992) has shown that health care workers spend 60 to 80% of their workday standing (see table 1). Belgian nurses were observed to spend approximately 10% of their workday bent over; Czechoslovakian nurses spent 11% of their workday positioning patients; and French nurses spent 16 to 24% of their workday in uncomfortable positions, such as stooping or squatting, or with their arms raised or loaded.
Table 1. Distribution of nurses’ time in three studies
|
Czechoslovakia |
Belgium |
France |
|
|
Authors |
Hubacova, Borsky and Strelka 1992* |
Malchaire 1992** |
Estryn-Béhar and |
|
Departments |
5 medical and surgical departments |
Cardiovascular surgery |
10 medical and |
|
Average time for the main postures and total distance walked by nurses: |
|||
|
Per cent working |
76% |
Morning 61% |
Morning 74% |
|
Including stooping, |
11% |
Morning 16% |
|
|
Standing flexed |
Morning 11% |
||
|
Distance walked |
Morning 4 km |
Morning 7 km |
|
|
Per cent working |
Three shifts: 47% |
Morning 38% |
Morning 24% |
Number of observations per shift:* 74 observations on 3 shifts. ** Morning: 10 observations (8 h); afternoon: 10 observations (8 h); night: 10 observations (11 h). *** Morning: 8 observations (8 h); afternoon: 10 observations (8 h); night: 9 observations (10-12 h).
In France, night-shift nurses spent somewhat more time sitting, but they end their shift by making beds and dispensing care, both of which involve work in uncomfortable positions. They are assisted in this by a nurses’ aide, but this should be contrasted with the situation during the morning shift, where these tasks are usually performed by two nurses’ aides. In general, nurses working day shifts spend less time in uncomfortable positions. Nurses’ aides were on their feet constantly, and uncomfortable positions, due largely to inadequate equipment, accounted for 31% (afternoon shift) to 46% (morning shift) of their time. Patient facilities in these French and Belgian teaching hospitals were spread out over large areas and consisted of rooms containing one to three beds. Nurses in these wards walked an average of 4 to 7 km per day.
Detailed ergonomic observation of entire workdays (Estryn-Béhar and Hakim-Serfaty 1990) is useful in revealing the interaction of the factors that determine quality of care and the manner in which work is performed. Consider the very different situations in a paediatric intensive care unit and a rheumatology ward. In paediatric resuscitation units, the nurse spends 71% of her time in patients’ rooms, and each patient’s equipment is kept on individual carts stocked by nurses’ aides. The nurses in this ward change location only 32 times per shift, walking a total of 2.5 km. They are able to communicate with physicians and other nurses in the adjoining lounge or nurses’ station through intercoms which have been installed in all the patients’ rooms.
By contrast, the nursing station in the rheumatology ward is very far from patients’ rooms, and care preparation is lengthy (38% of shift time). As a result, the nurses spend only 21% of their time in patients’ rooms and change location 128 times per shift, walking a total of 17 km. This clearly illustrates the interrelationship between physical strain, back problems and organizational and psychological factors. Because they need to move rapidly and get equipment and information, nurses only have time for hallway consultations—there is no time to sit while dispensing care, listen to patients and give patients personalized and integrated responses.
Continuous observation of 18 Dutch nurses in long-term-stay wards revealed that they spent 60% of their time performing physically demanding work with no direct contact with their patients (Engels, Senden and Hertog 1993). Housekeeping and preparation account for most of the 20% of the time described as spent in “slightly hazardous” activities. In all, 0.2% of shift time was spent in postures requiring immediate modification and 1.5% of shift time in postures requiring rapid modification. Contact with patients was the type of activity most frequently associated with these hazardous postures. The authors recommend modifying patient-handling practices and other less hazardous but more frequent tasks.
Given the physiological strain of the work of nurses’ aides, continuous measurement of heart rate is a useful complement to observation. Raffray (1994) used this technique to identify arduous housekeeping tasks and recommended not restricting personnel to this type of task for the whole day.
Electro-myographical (EMG) fatigue analysis is also interesting when body posture must remain more or less static—for example, during operations using an endoscope (Luttman et al. 1996).
Influence of architecture, equipment and organization
The inadequacy of nursing equipment, particularly beds, in 40 Japanese hospitals was demonstrated by Shindo (1992). In addition, patients’ rooms, both those lodging six to eight patients and single rooms reserved for the very ill, were poorly laid out and extremely small. Matsuda (1992) reported that these observations should lead to improvements in the comfort, safety and efficiency of nursing work.
In a French study (Saurel 1993), the size of patient rooms was problematic in 45 of 75 medium- and long-term-stay wards. The most common problems were:
- lack of space (30 wards)
- difficulty in manoeuvring patient-transfer gurneys (17)
- inadequate space for furniture (13)
- the need to take beds out of the room to transfer patients (12)
- difficult access and poor furniture layout (10)
- doors that were too small (8)
- difficulty moving between beds (8).
The mean available area per bed for patients and nurses is at the root of these problems and decreases as the number of beds per room increases: 12.98 m2, 9.84 m2, 9.60 m2, 8.49 m2 and 7.25 m2 for rooms with one, two, three, four and more than four beds. A more accurate index of the useful area available to personnel is obtained by subtracting the area occupied by the beds themselves (1.8 to 2.0 m2) and by other equipment. The French Department of Health prescribes a useful surface area of 16 m2 for single rooms and 22 m2 for double rooms. The Quebec Department of Health recommends 17.8 m2 and 36 m2, respectively.
Turning to factors favouring the development of back problems, variable-height mechanisms were present on 55.1% of the 7,237 beds examined; of these, only 10.3% had electric controls. Patient-transfer systems, which reduce lifting, were rare. These systems were systematically used by 18.2% of the 55 responding wards, with over half the wards reporting using them “rarely” or “never”. “Poor” or “rather poor” manoeuvrability of meal carts was reported by 58.5% of 65 responding wards. There was no periodic maintenance of mobile equipment in 73.3% of 72 responding wards.
In almost half the responding wards, there were no rooms with seats that nurses could use. In many cases, this appears to have been due to the small size of the patient rooms. Sitting was usually possible only in the lounges—in 10 units, the nursing station itself had no seats. However, 13 units reported having no lounge and 4 units used the pantry for this purpose. In 30 wards, there were no seats in this room.
According to statistics for 1992 provided by the Confederation of Employees of the Health Services Employees of the United Kingdom (COHSE), 68.2% of nurses felt that there were not enough mechanical patient lifts and handling aides and 74.5% felt that they were expected to accept back problems as a normal part of their work.
In Quebec, the Joint Sectoral Association, Social Affairs Sector (Association pour la santé et la sécurité du travail, secteur afffaires sociales, ASSTAS) initiated its “Prevention-Planning-Renovation-Construction” project in 1993 (Villeneuve 1994). Over 18 months, funding for almost 100 bipartite projects, some costing several million dollars, was requested. This programme’s goal is to maximize investments in prevention by addressing health and safety concerns early in the design stage of planning, renovation and design projects.
The association completed the modification of the design specifications for patient rooms in long-term-care units in 1995. After noting that three-quarters of occupational accidents involving nurses occur in patient rooms, the association proposed new dimensions for patients’ rooms, and new rooms must now provide a minimum amount of free space around beds and accommodate patient lifts. Measuring 4.05 by 4.95 m, the rooms are more square than the older, rectangular rooms. To improve performance, ceiling-mounted patient lifts were installed, in collaboration with the manufacturer.
The association is also working on the modification of construction standards for washrooms, where many occupational accidents also occur, although to a lesser extent than in the rooms themselves. Finally, the feasibility of applying anti-skid coatings (with a coefficient of friction above the minimum standard of 0.50) on floors is being studied, since patient autonomy is best promoted by providing a non-skid surface on which neither they nor nurses can slip.
Evaluation of equipment that reduces physical strain
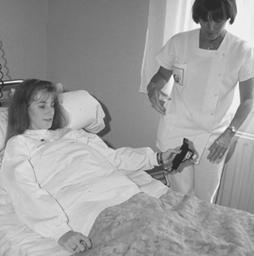
Proposals for improving beds (Teyssier-Cotte, Rocher and Mereau 1987) and meal carts (Bouhnik et al. 1989) have been formulated, but their impact is too limited. Tintori et al. (1994) studied adjustable-height beds with electric trunk-lifts and mechanical mattress-lifts. The trunk-lifts were judged satisfactory by the staff and patients, but the mattress-lifts were very unsatisfactory, since adjusting the beds required more than eight pedal strokes, each of which exceeded standards for foot force. Pushing a button located close to the patient’s head while talking to her or him is clearly preferable to pumping a pedal eight times from the foot of the bed (see figure 1). Because of time constraints, the mattress lift was often simply not used.
Figure 1. Electronically-operated trunk-lifts on beds effectively reduce lifting accidents
B. Floret
Van der Star and Voogd (1992) studied health care workers caring for 30 patients in a new prototype of bed over a period of six weeks. Observations of the workers’ positions, the height of work surfaces, physical interaction between nurses and patients and the size of the work space were compared to data collected on the same ward over a seven-week period prior to the introduction of the prototype. Use of the prototypes reduced the total time spent in uncomfortable positions while washing patients from 40% to 20%; for bed-making the figures were 35% and 5%. Patients also enjoyed greater autonomy and often changed positions on their own, raising their trunks or legs by means of electric control buttons.
In Swedish hospitals, each double room is equipped with ceiling-mounted patient lifts (Ljungberg, Kilbom and Goran 1989). Rigorous programmes such as the April Project evaluate the interrelation of working conditions, work organization, the establishment of a back school and the improvement of physical fitness (Öhling and Estlund 1995).
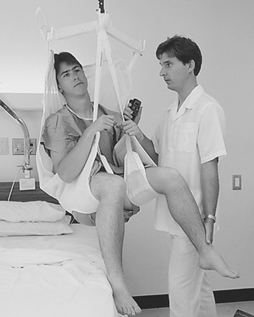
In Quebec, ASSTAS developed a global approach to the analysis of working conditions causing back problems in hospitals (Villeneuve 1992). Between 1988 and 1991, this approach led to modifications of the work environment and equipment used in 120 wards and a 30% reduction in the frequency and severity of occupational injuries. In 1994, a cost-benefit analysis performed by the association demonstrated that the systematic implementation of ceiling-mounted patient lifts would reduce occupational accidents and increase productivity, compared to the continued use of mobile, ground-based lifts (see figure 2).
Figure 2. Using ceiling-mounted patient lifts to reduce lifting accidents
Accounting for individual variation and facilitating activity
The female population in France is generally not very physically active. Of 1,505 nurses studied by Estryn-Béhar et al. (1992), 68% participated in no athletic activity, with inactivity more pronounced among mothers and unskilled personnel. In Sweden, fitness programmes for hospital personnel have been reported to be useful (Wigaeus Hjelm, Hagberg and Hellstrom 1993), but are feasible only if potential participants do not end their work day too tired to participate.
The adoption of better work postures is also conditioned by the possibility of wearing appropriate clothing (Lempereur 1992). The quality of shoes is particularly important. Hard soles are to be avoided. Anti-skid soles prevent occupational accidents caused by slips and falls, which in many countries are the second-leading cause of accidents leading to work absence. Ill-fitting overshoes or boots worn by operating room personnel to minimize the build-up of static electricity may be a hazard for falls.
Slips on level floors can be prevented by using low-slip floor surfaces that require no waxing. The risk of slips, particularly at doorways, can also be reduced by using techniques that do not leave the floor wet for long. The use of one mop per room, recommended by hygiene departments, is one such technique and has the additional advantage of reducing the handling of buckets of water.
In Vasteras County (Sweden), the implementation of several practical measures reduced painful syndromes and absenteeism by at least 25% (Modig 1992). In the archives (e.g., record or file rooms), ground- and ceiling-level shelves were eliminated, and an adjustable sliding board on which personnel can take notes while consulting the archives was installed. A reception office equipped with movable filing units, a computer and a telephone was also constructed. The height of the filing units is adjustable, allowing employees to adjust them to their own needs and facilitating the transition from sitting to standing during work.
Importance of “anti-lifting”
Manual patient-handling techniques designed to prevent back injuries have been proposed in many countries. Given the poor results of these techniques that have been reported to date (Dehlin et al. 1981; Stubbs, Buckle and Hudson 1983), more work in this area is needed.
The department of kinesiology of the University of Groningen (Netherlands) has developed an integrated patient-handling programme (Landewe and Schröer 1993) consisting of:
- recognition of the relationship between patient-handling and back strain
- demonstration of the value of the “anti-lifting” approach
- sensitization of nursing students throughout their studies to the importance of avoiding back strain
- the use of problem-resolution techniques
- attention to implementation and evaluation.
In the “anti-lifting” approach, the resolution of problems associated with patient transfers is based on the systematic analysis of all aspects of transfers, especially those related to patients, nurses, transfer equipment, teamwork, general working conditions and environmental and psychological barriers to the use of patient lifts (Friele and Knibbe 1993).
The application of European standard EN 90/269 of 29 May 1990 on back problems is an example of an excellent starting point for this approach. Besides requiring employers to implement appropriate work organization structures or other appropriate means, particularly mechanical equipment, to avoid manual handling of loads by workers, it also emphasizes the importance of “no-risk” handling policies that incorporate training. In practice, the adoption of appropriate postures and handling practices depends on the amount of functional space, presence of appropriate furniture and equipment, good collaboration on work organization and quality of care, good physical fitness and comfortable work clothing. The net effect of these factors is improved prevention of back problems.